Long COVID Explained: The Symptoms and Why They Stick Around
Last updated: January 15, 2024
Millions of individuals who have tested positive for COVID-19 continue to experience ongoing health issues, clinically known as long COVID. If you’re one of these people, the Aviv team is here with research-backed information on what this means and what you can do.
While there is still uncertainty surrounding COVID-19 complications and their long-term side effects, there have been extensive studies conducted that offer insight into:
- Post COVID symptoms
- How long COVID can impact your body and lifestyle
- Treatment methods that can help mitigate long-haul COVID effects
Below, we provide all the details you need to attain a holistic understanding of how long COVID impacts your body and promising treatment plans that can help you get back to optimal health. As you’re reading through this, keep in mind:
- Each person has a unique experience with COVID-19.
- Therefore, speaking with a doctor is an essential first step.
- Several alternative terms are used for long COVID, such as post-COVID, long-haul COVID, post-acute COVID, and chronic COVID.
How the CDC and WHO Define Long COVID
- The Centers for Disease Control and Prevention (CDC) defines long COVID as a condition where individuals experience long-term effects of COVID-19.
- The World Health Organization (WHO) defines long COVID as persistent symptoms more than 3 months after the acute infection, that continue, not relapse, that have been reoccurring and there is no other explanation for those symptoms.
- Anyone who has been infected with COVID-19 can develop long COVID. Approximately 30% of COVID-19 patients report having symptoms of long-haul COVID.
The numbers of people affected long term are high
The WHO had a definition of long COVID over two years ago. That means, from nearly the beginning, these health organizations studying the virus were seeing long-term side effects and symptoms of impairment from having COVID-19.
You aren’t alone if you don’t feel like yourself after having COVID-19.
- Approximately 30% of COVID-19 patients report having symptoms of long-haul COVID.
- 20-50% of patients with 1 or more features 3-6 months post COVID, receive a long COVID diagnosis.
- 11-20% of children have lingering symptoms at 14 weeks post COVID.
For a comprehensive understanding of what long-haul COVID is, let’s flesh out the differences between COVID and long COVID:
Acute COVID:
- Individuals experience COVID-19 symptoms for up to four weeks, starting from the onset of illness.
- Subacute is where COVID-19 symptoms are noticed up to 12 weeks, and the virus can still be found in the body.
Long COVID:
- Individuals experience COVID-19 symptoms for an average of three months from the onset of illness.
- Long-haul COVID symptoms may begin after initial recovery from acute COVID or persist from the initial illness.
- Long COVID symptoms cannot be explained by an alternative diagnosis.
Understanding the Symptoms of Long-Haul COVID
The Aviv medical staff primarily explores the four key areas from this long-haul COVID symptoms list to diagnose long COVID.
Physical Symptoms:
- Fatigue
- Dyspnea (labored breathing)
- Chest pain or tightness
- Cough
- Dysgeusia (loss of taste)
- Anosmia (loss of smell)
- Joint or muscle pain
Cognitive & Psychological Symptoms:
- Memory decline
- Attention and concentration difficulties
- Brain fog
- Anxiety
- Depression
- Sleep disturbances
- Headaches
- Generalized disabling pain
- Lung Symptoms
- Shortness of breath
- Chest pain or tightness
Cardiac Symptoms:
- Myocarditis (inflammation of heart muscles)
- Heart palpitations
- Shortness of breath
- Elevated blood pressure
- Drops in oxygen saturation
If you are experiencing long COVID symptoms,
contact our team of certified medical professionals today – click here.
The Hard Truth: Long COVID & Brain Injuries
COVID-19 essentially impacts the brain. This is why the majority of long COVID symptoms are cognitive and may lead to brain injuries, depending on how severely your body gets affected by the virus.
According to Dr. Mohammed Elimar, MD, FACP, although there are no patterns between the severity of COVID-19 and the likelihood of receiving long COVID, there are patterns between:
- Where the virus attacks in the brain
- How that location in the brain impacts long COVID symptoms
Here are four ways that connection can manifest:
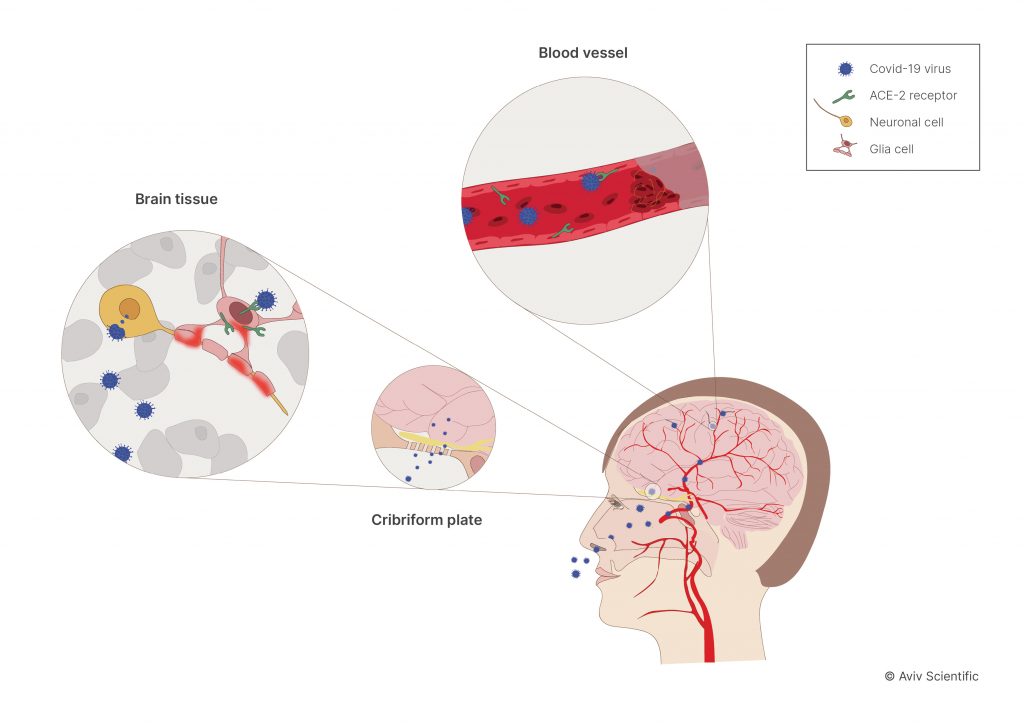
1. Direct Brain Invasion
The COVID-19 virus travels through the nose, into the olfactory sensory neurons, and into the frontal lobe of your brain called the insula. The olfactory neurons manage taste and smell, while the insula oversees memory and executive function. Depending on where the virus attacks and the level of damage it creates, an individual may experience prolonged COVID symptoms.
For example, when the virus significantly attacks your olfactory nerves, this may induce a loss of taste and smell. This is why these symptoms are such a strong indicator of the virus.
2. Blood Vessel Injury
Studies show COVID-19 can destroy blood vessels that feed blood to the brain. As the virus circulates throughout your bloodstream, the inner blood vessel lining is susceptible to damage. When the inner lining deteriorates, this allows the virus to: Seep into the tissues, or inhibit blood flow to the brain. Both can cause brain injuries. And depending on where those injuries occur, specific brain functions (memory, concentration, etc.) may decline more rapidly than normal.
3. Dysregulated Immune Response
Damage to the inner blood vessel lining can also inhibit the growth of cells—the exact opposite of what our immune system should be doing. Dysregulated immune responses are common in those with severe cases of COVID-19.
When the body cannot adequately produce a normal immune response, it either: Underreacts to foreign invaders, causing viruses to spread quickly; or oerreacts to foreign invaders, causing the immune cells to attack even healthy cells, tissues, and organs.
4. Cellular Dysfunction
On a cellular level, COVID-19 can affect metabolic function through the mitochondria. This cell damage slows down the body’s response rate to infection, leading to high inflammatory conditions.
So how long will patients have to deal with COVID symptoms?
According to Dr. Mohammed Elimar, MD, FACP, the answer isn’t available.
But a key guiding factor is the extent of blood vessel damage.
Dr. Elimar further explains:
“There’s still a lot to learn about how [mitochondrial dysfunction] will last but it will probably be tied to the level of microvascular change or blood vessel damage. The more blood vessel damage you have, the more [long COVID symptoms] you’re likely going to have. Also, the amount of real estate that those microvascular changes are occupying will probably dictate how long [symptoms] will last.”
Aviv Clinics’ Treatment for Long COVID Symptoms
Long COVID is a complex disease.
Finding a treatment plan that will work for you may take some time.
Because there is no one-size-fits-all approach, speaking with a medical professional is essential.
The right physician will take a holistic approach. Due to the complexity of long COVID, it’s important to find a treatment program that:
- Is rooted in data and research
- Offers a comprehensive assessment process
- Connects you with a diverse medical team
Aviv Clinic’s team of certified physicians achieves all of the above to ensure you’re being provided with a tailored treatment plan that works for you. We connect our patients with a team of physicians, neuropsychologists, physiotherapists, nurses, and more to provide a multidisciplinary health plan – The Aviv Medical Program.
Our post-COVID symptom treatment plan can be broken down into three parts:
- In-depth medical assessment:
Leveraging advanced brain imaging, our clinical team conducts physical, cognitive, and neurological exams to gain a thorough understanding of your health. - Tailored treatment program:
Based on your assessment, our medical team crafts a personalized treatment plan, based on the results of your assessments, that includes hyperbaric oxygen therapy sessions, brain and physical training and a nutritional regimen designed to maximize the body’s healing process. - Post-treatment assessment:
Our team initiates another round of tests to assess your progress and unique findings on any cognitive and physical improvements.
Watch Patrick’s Successful Journey in Fighting Long COVID
First Long COVID treatment backed by clinical trials – help heal the brain to reduce or eliminate the symptoms of long COVID
The Aviv Medical Program is backed by extensive clinical research.
The most recent study confirmed that the COVID-19 virus can cause chronic brain injury affecting regions of the brain responsible for cognitive function, mental status and pain interpretation.
In the published study, patients treated with the Aviv protocol had significant improvement in their global cognitive function and cognitive improvement in the damaged brain regions responsible for attention and executive function. Significant improvement was also demonstrated in the energy domain, sleep, psychiatric symptoms and pain interference. The beneficial effects of the unique treatment protocol can be attributed to neuroplasticity and increased brain perfusion in regions associated with cognitive and emotional roles.
Read more about the Aviv Medical Program for Long COVID
Dr. Shai Efrati of summarizes the results of a study by saying:
“HBOT can induce neuroplasticity and improve cognitive performance, psychiatric state, assist with fatigue, aid sleep and relieve pain symptoms for patients suffering from post covid 19 condition. The beneficial effect can be attributed to increased brain perfusion and brain plasticity in regions associated with cognitive and emotional roles. HBOT can repair brain network connectivity and activity, and improve cardiac functions in post covid patients suffering from reduced GLS.”
WebMD recently published the research of Dr. Efrati, noting the clinical trial that began in December 2020 shows great potential for Long COVID patients whose issues are connected to brain tissue damage.
Maximize Your Health and Performance with Aviv
Though COVID-19 may have brought ongoing health challenges, the Aviv team is here to help you and your loved ones get back to optimal health. Aviv delivers a personalized protocol to enhance your mind and body and feel like yourself again.
Learn more about our team, contact our clinic to schedule a free phone consultation. Maximizing your health and performance begins with Aviv.